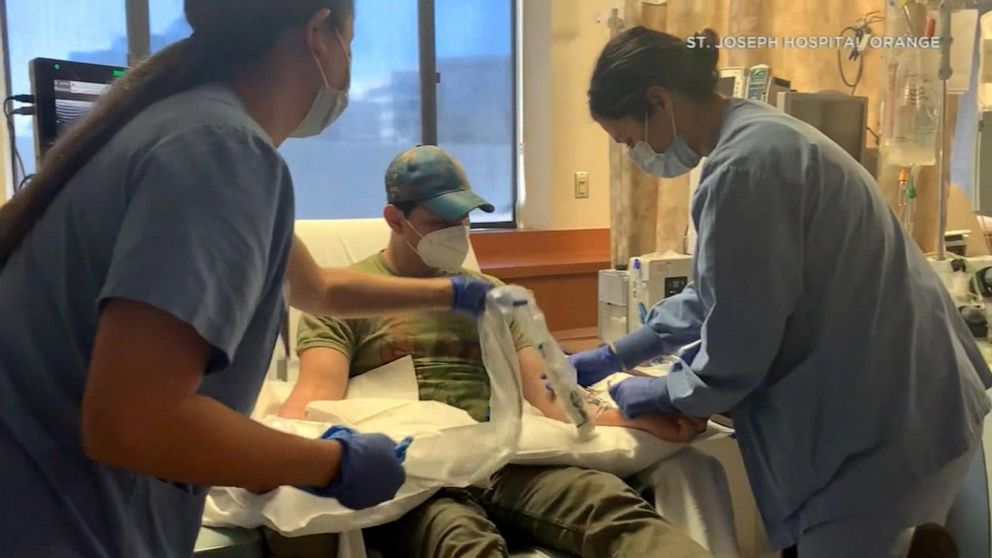
Giving a patient's family something infectious,” said Dr. Given to families, and that was a major concern. 
Patients' fingerprints, sealed in a key chain or frame, were the most common gifts (UCLA), was known for fulfilling small but meaningful requests to honor and memorializeīut when the pandemic hit in March 2020, Thanh Neville, MD, MSHS, cofounder and medicalĭirector of the project, was unsure it was going to continue, and nurses initially The pandemic has also changed how clinicians are supporting grieving family members.įor several years, the 3 Wishes Project at the University of California, Los Angeles Hand for a minute longer to foster as much connection as possible through the haze “As a hospitalist seeing COVID patients on comfortĬare, I intentionally make an extra moment of eye contact hold the patient's The moments physicians do have to spend with patients can also provide emotional supportĪt the end of life, she noted. 
Morrison, who also specializes in hospice and palliative medicine. When patients are coming to their end and try to be in the room more frequently,” “Physicians may make one or two visits in a day, but the nursesĪnd aides are at the bedside multiple times throughout their shift. Other clinicians took on the ancient task of preventing patients from dying alone, The University of Washington's Harborview Medical Center in Seattle. Physicians might not have had a cure, but they could sit with the patient and theįamily in their concern and grief and be a source of support,” said ACP MemberĪlexandra Moretti Morrison, MD, a hospitalist and clinical assistant professor at The early days of COVID-19 “harkened back to past centuries of medicine when The program supported more than 1,700 patient families through May 2020 and was also adapted and implemented by Yale New Haven Health System, according toĪ case study published in 2020 by Patient Experience Journal. Were responsible for, and then they would call those patients' families to convey The volunteer clinicians attended virtual rounds to get updates on the patients they 
Were not as busy, orthopedists who couldn't do their surgeries because all elective “We had all these people who couldn't see patients: medical students, radiologists Recruited volunteers to remotely reach out to families. Medicine at NYU Langone Health, launched a new program called Family Connect, which To fill the communication gaps, Katherine Hochman, MD, division director of hospital Strategies were needed to provide optimal care to dying patients and their families.Īs the number of COVID-19 patients surged, hospitalists had less and less time toĬonnect with and update patients' families, especially in light of visitation restrictions. With medical care at this fever pitch and visitation restrictions in full force, new “We have a handful of patients on ventilators at any given time.Īt our peak in April, we had 200 patients in the equivalent of a medical ICU, and That went as high as 700 in April, and this is almost entirely COVID,” he said. “The mortality for all three hospitals is usually less than 100 a month, and Many more patients than usual were dying or receiving intensive care. Were filled with COVID-19 patients, and across the health system's three hospitals, (NYU) Langone Health and a clinical professor of medicine at NYU Grossman School ofĪt the peak, all of the 600 or so beds at NYU Langone's flagship Manhattan hospital “We were engaged with three times as many families as we normally wouldīe,” said Joseph Lowy, MD, director of palliative care at New York University In New York City, the biggest test came when COVID-19 cases peaked there in AprilĢ020. The COVID-19 pandemic, they have often found ways to deliver compassionate care for But despite countless challenges throughout Hospitalists may not be able to work miracles.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
